
Latest In Conference Reporter
More in Expert Perspectives

Oncology
Evaluating Patient Risk Factors When Diagnosing Myelofibrosis

Oncology
Expert Perspectives in Gastroenteropancreatic Neuroendocrine Tumors to Cover Key Topics in GEP-NETs Treatment

Oncology
Optimizing Allogeneic Hematopoietic Stem Cell Transplant and Relapse Management in Acute Myeloid Leukemia
Dermatology
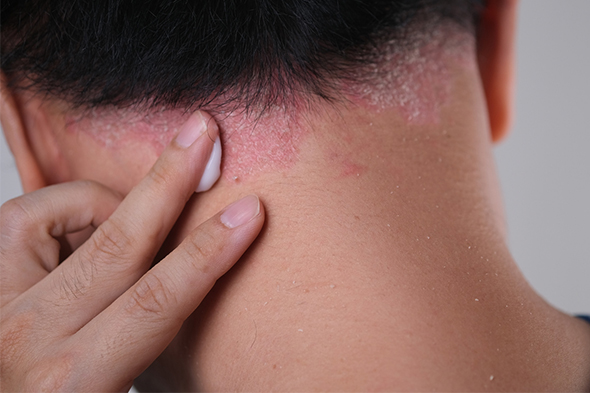
Real-World Results on Long-term Adherence to Plaque Psoriasis Treatment
Oncology
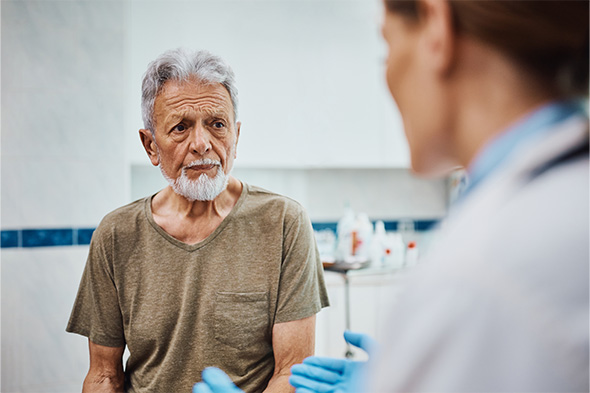
Treating Older Patients With Newly Diagnosed Acute Myeloid Leukemia
Load More















