
Latest In Conference Reporter
More in Expert Perspectives

Oncology
Evaluating Patient Risk Factors When Diagnosing Myelofibrosis

Gastroenteropancreatic Neuroendocrine Tumors
Expert Perspectives in Gastroenteropancreatic Neuroendocrine Tumors to Cover Key Topics in GEP-NETs Treatment

Oncology
Optimizing Allogeneic Hematopoietic Stem Cell Transplant and Relapse Management in Acute Myeloid Leukemia
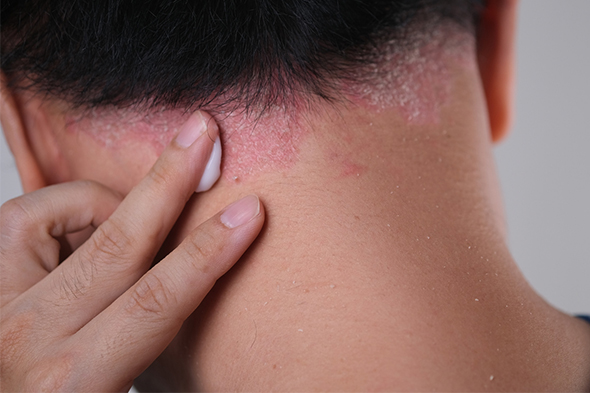
Dermatology
Real-World Results on Long-term Adherence to Plaque Psoriasis Treatment
Oncology
Treating Older Patients With Newly Diagnosed Acute Myeloid Leukemia
Load More















